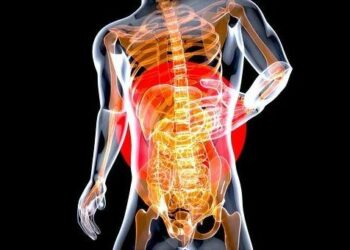
Gastroparesis impacts how the abdomen strikes meals into the intestines and results in bloating, nausea, and heartburn. When diabetes causes the situation, medical doctors name it diabetic gastroparesis.
On this article, we offer an summary of diabetic gastroparesis, together with its causes, signs, problems, and coverings.

Diabetic gastroparesis refers to instances of the digestive situation gastroparesis that diabetes causes.
Throughout regular digestion, the abdomen contracts to assist break down meals and transfer it into the small gut. Gastroparesis disrupts the abdomen’s contraction, which may interrupt digestion.
Diabetes may cause gastroparesis because of its results on the nervous system.
Each type 1 diabetes and type 2 diabetes may cause nerve injury. One of many nerves diabetes might injury is the vagus nerve. The vagus nerve controls the motion of meals via the abdomen.
When the vagus nerve experiences injury, the muscle tissues within the abdomen and different components of the digestive tract usually are not in a position to operate correctly. When this occurs, meals can’t transfer as shortly via the digestive system.
Gastroparesis is also called delayed gastric emptying.
Indicators and signs of gastroparesis fluctuate in severity from individual to individual and should embody any mixture of the next:
- nausea and vomiting, significantly of undigested meals
- heartburn
- feeling full after consuming little or no
- lack of urge for food
- unintentional weight reduction
- bloating
- unstable blood sugar ranges
- gastroesophageal reflux
- abdomen spasms
Some individuals with diabetes are at larger threat of creating gastroparesis than individuals with out diabetes.
Danger elements for creating diabetic gastroparesis embody:
- having kind 1 diabetes
- having kind 2 diabetes for longer than 10 years
- having coexisting autoimmune ailments
- having a historical past of sure gastric surgical procedures
Gastroparesis is
Individuals who have had sure cancer remedies, reminiscent of radiation therapy across the chest or abdomen space, are additionally extra prone to develop gastroparesis.
Gastroparesis makes it tougher for an individual with diabetes to handle their blood sugar ranges.
Generally, the abdomen of an individual with gastroparesis might take a really very long time to empty the meals into the gut for absorption. Different instances, the abdomen might cross the meals in a short time.
This unpredictability makes it tough for somebody with diabetes to know when to take insulin, which means that their blood sugar ranges might get too excessive or too low at instances.
When blood sugar ranges are too excessive it places an individual with diabetes at larger threat of the next:
When blood sugar ranges drop too low, an individual with diabetes might expertise the next problems:
- shakiness
- diabetic coma from low blood sugar
- lack of consciousness
- seizures
Different problems from diabetic gastroparesis can embody:
- malnutrition
- bacterial infections
- indigestible plenty, often known as bezoars, which may trigger abdomen obstruction
- electrolyte imbalance
- tears within the esophagus from power vomiting
- inflammation of the esophagus which will trigger issue swallowing
If a physician suspects an individual with diabetes has gastroparesis, they’ll sometimes order a number of of the next checks to verify the analysis.
Barium X-ray
A health care provider might begin with a barium X-ray to test for gastroparesis. For a barium X-ray, an individual will quick for 12 hours, drink a liquid containing barium, after which have an belly X-ray. The barium will coat the abdomen to make it seen on X-ray.
Often, an individual who has fasted previous to this check has an empty abdomen. Nevertheless, somebody with gastroparesis should have some meals of their abdomen.
Barium beefsteak check
The barium beefsteak check includes an individual consuming meals that accommodates barium after which having imaging checks whereas the meal digests. A health care provider will watch the individual’s abdomen by way of imaging to see how lengthy it takes for meals to depart.
Radioisotope gastric-emptying scan
Much like the barium beefsteak check, the radioisotope gastric-emptying scan includes an individual consuming meals that accommodates a radioactive compound earlier than they’ve an imaging check.
Gastric manometry
A gastric manometry measures the exercise of the muscle tissues within the abdomen.
Throughout a gastric manometry, a physician will insert a slim tube via an individual’s throat into their abdomen. The tube features a gadget that measures the abdomen’s exercise because it digests meals. The measurements present how properly the abdomen is functioning.
Different checks
Moreover, a physician who suspects diabetic gastroparesis might order any of the next checks:
- Blood checks to test for dietary deficiencies and electrolyte imbalances which might be widespread with gastroparesis.
- Imaging of the gallbladder, kidneys, and pancreas to rule out gallbladder issues, kidney illness, or pancreatitis as causes.
- An higher endoscopy to test for abnormalities within the construction of the abdomen.
Managing blood sugar ranges is an important a part of treating diabetic gastroparesis.
Most medical doctors will advise an individual with diabetic gastroparesis to test their blood sugar ranges extra ceaselessly than somebody with diabetes who doesn’t have gastroparesis. Extra frequent blood sugar checks may help the person and their physician higher tailor their therapy.
Therapy can embody any mixture of the next:
- altering the dosage and timing of insulin
- oral drugs for gastroparesis, together with medicine that stimulate the abdomen muscle tissues and drugs for nausea
- avoiding medicine which will delay gastric emptying, reminiscent of opiates
- adjustments in weight-reduction plan and consuming habits
In some instances, an individual with diabetic gastroparesis might have a feeding tube or intravenous nutrition. Docs solely suggest this if the individual can’t handle their blood sugar or the gastroparesis may be very extreme.
When a feeding tube is required, it’s going to bypass the abdomen fully, placing vitamins immediately into the gut. This helps maintain blood sugar ranges secure. In lots of cases, feeding tubes are non permanent.
Many medical doctors will suggest an individual with diabetic gastroparesis make sure dietary adjustments, together with:
- consuming frequent, smaller meals as a substitute of three bigger meals every day
- limiting high-fiber meals, reminiscent of broccoli, which take longer to digest
- sticking to primarily low-fat meals
- consuming well-cooked greens as a substitute of uncooked greens
- avoiding alcohol and carbonated drinks
A health care provider or nutritionist might suggest an individual with diabetic gastroparesis eats sure meals, together with:
- lean meats, reminiscent of lean cuts of beef or pork
- skinless poultry with a low-fat preparation technique (not fried)
- low-fat fish
- tofu
- eggs
- tomato sauce
- cooked carrots and mushrooms
- skinless candy potatoes
- applesauce with no added sugar
- low-fat milk or yogurt
Additionally, a physician or nutritionist will possible suggest that an individual with diabetic gastroparesis make some adjustments round meal instances, reminiscent of taking a stroll after consuming to advertise digestion. Likewise, many medical doctors might recommend ready no less than two hours after consuming to put down.
A complete evaluate within the journal
Individuals with diabetic gastroparesis are additionally extra prone to expertise eye injury, kidney injury, and coronary heart illness than these with diabetes alone. This elevated threat of problems might elevate an individual’s threat of early demise because of diabetes-related causes.
The probability of problems and total outlook for an individual with diabetic gastroparesis will fluctuate between people. Usually, individuals can enhance their outlook by studying the right way to greatest handle their blood sugar ranges every day.